Psoriasis Vulgaris
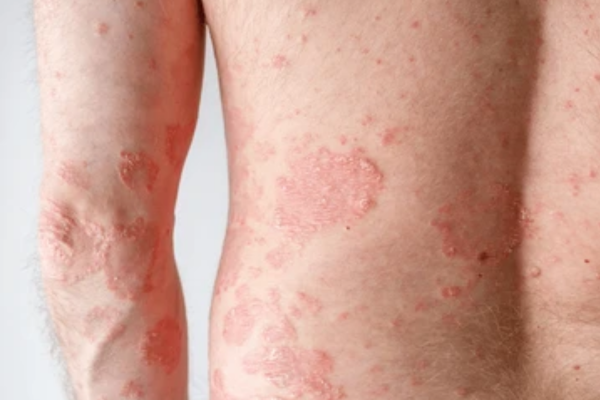
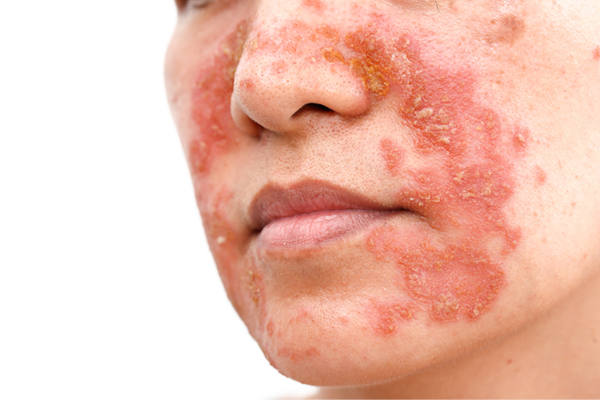
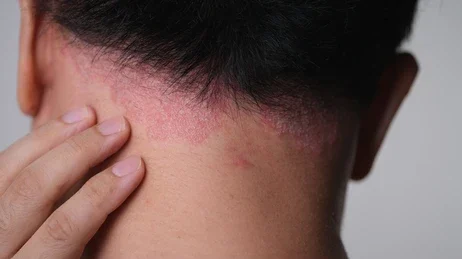
Psoriasis vulgaris, commonly known as psoriasis, is a chronic autoimmune condition that affects the skin. It results in the rapid turnover of skin cells, leading to the formation of red, thickened patches with silvery scales known as plaques. Psoriasis can occur anywhere on the body but most often affects the elbows, knees, scalp, and lower back.
Understanding the triggers, symptoms, and seeking dermatological care are essential for effectively managing psoriasis.
Possible Causes of Acne
Psoriasis vulgaris develops due to a combination of genetic, immune system, and environmental factors:
- Genetic Predisposition: Family history plays a significant role in the development of psoriasis. Certain genes are associated with an increased risk of developing the condition.
- Immune System Dysfunction: In psoriasis, the immune system mistakenly attacks healthy skin cells, triggering inflammation and excessive skin cell turnover.
- Triggers: Various factors can trigger or exacerbate psoriasis flare-ups, including stress, infections (such as streptococcal throat infections), certain medications (such as lithium and beta-blockers), and injuries to the skin (Koebner phenomenon).
- Environmental Factors: Cold weather, dry climate, and excessive sun exposure can worsen symptoms in some individuals with psoriasis.
Symptoms and Diagnosis
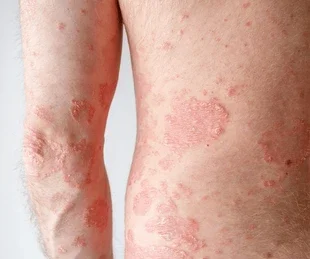
Psoriasis vulgaris is characterized by:
- Red, Thickened Skin: Plaques of red, inflamed skin covered with silvery scales.
- Itching and Discomfort: Plaques may be itchy or painful, particularly if they crack and bleed.
- Nail Changes: Psoriasis can affect fingernails and toenails, causing pitting, discoloration, and separation from the nail bed.
Diagnosis is typically based on a physical examination and may involve a skin biopsy to confirm the diagnosis and rule out other skin conditions.
Importance of Visiting Dermatologist
- Accurate Diagnosis: Dermatologists specialize in diagnosing psoriasis and differentiating it from other skin conditions that may appear similar, such as eczema or seborrheic dermatitis.
- Tailored Treatment Plans: Dermatologists develop personalized treatment plans based on the type, severity, and location of psoriasis plaques. Treatment options may include topical treatments (such as corticosteroids and vitamin D analogy), phototherapy (light therapy), systemic medications (such as methotrexate or biologics), and lifestyle modifications.
- Monitoring and Management: Regular visits to a dermatologist allow for ongoing assessment of psoriasis symptoms and treatment effectiveness. Dermatologists can adjust treatment plans as needed to achieve optimal skin clearance and minimize flare-ups.
- Education and Support: Dermatologists provide valuable education on psoriasis triggers, symptom management strategies, and the importance of skincare routines. They also offer support to help patients cope with the emotional and psychological impact of living with a chronic skin condition.
Need Any Help
Request A Consultation And Price Estimate

Atopic Dermatitis / Eczema
Atopic Dermatitis, commonly known as eczema, is a chronic skin condition characterized by inflamed, itchy, and red patches on the skin. It is most common in children but can occur at any age. The condition tends to flare periodically and then subside. While the exact cause of atopic dermatitis is unknown, it is believed to involve a combination of genetic and environmental factors.
Possible Causes of Atopic Dermatitis
- Genetic Factors: Family history of eczema, allergies, or asthma increases the likelihood of developing atopic dermatitis.
- Immune System Dysfunction: An overactive immune system can cause the skin to become inflamed and itchy.
- Skin Barrier Defects: Mutations in the gene responsible for producing filaggrin, a protein that helps maintain the skin’s barrier function, can lead to dry and more easily irritated skin.
- Environmental Triggers: Exposure to allergens, irritants, extreme temperatures, and certain fabrics can trigger or worsen symptoms.
- Microbial Factors: An imbalance in the skin microbiome, particularly the overgrowth of Staphylococcus aureus bacteria, can exacerbate the condition.
Symptoms and Diagnosis
- Symptoms:
- Itching: Intense itching, especially at night.
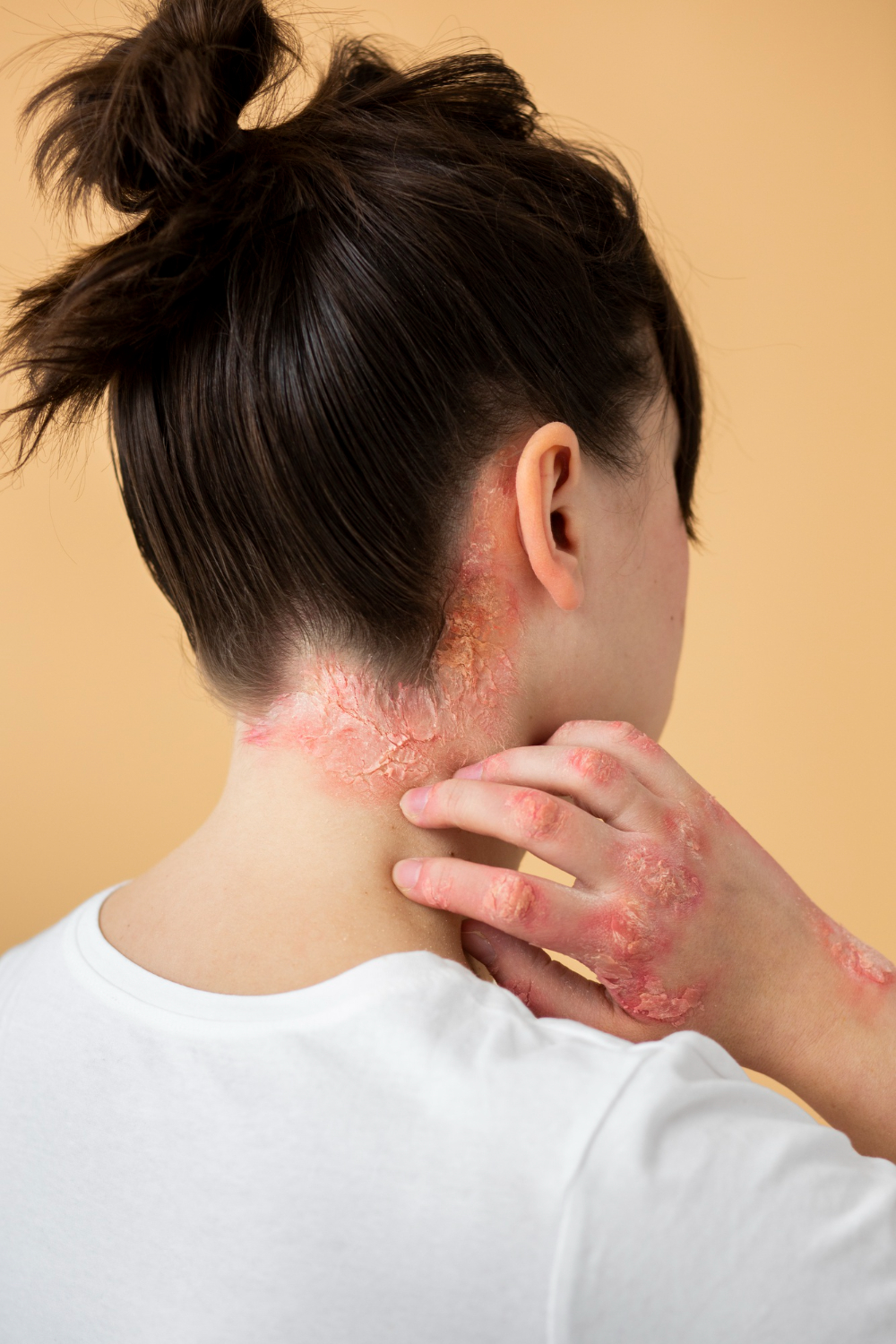
- Red or Brownish-Gray Patches: Common on the hands, feet, ankles, wrists, neck, upper chest, eyelids, and inside the bend of the elbows and knees.
- Small, Raised Bumps: These may leak fluid and crust over when scratched.
- Thickened, Cracked, or Scaly Skin: Chronic scratching can cause the skin to become thickened and leathery.
- Diagnosis: Dermatologists diagnose atopic dermatitis through a thorough examination of the skin and a review of the patient’s medical history. In some cases, allergy tests may be performed to identify potential triggers.

Importance of Visiting a Dermatologist at DermaLinks
- Accurate Diagnosis: Dermatologists can differentiate atopic dermatitis from other skin conditions with similar symptoms, such as psoriasis or contact dermatitis.
- Comprehensive Treatment Plans: Dermatologists can develop individualized treatment plans that address the specific needs and triggers of each patient. Common treatment plans include: Topical treatments, Systemic Treatments, Phototherapy, Lifestyle & Home remedies
- Access to Prescription Treatments: Dermatologists can prescribe stronger medications, such as topical corticosteroids, calcineurin inhibitors, and systemic treatments, which are not available over the counter.
- Monitoring and Managing Side Effects: Regular follow-ups with a dermatologist ensure that treatments are effective and any side effects are promptly addressed.
- Education and Support: Dermatologists can provide valuable information on managing the condition, avoiding triggers, and maintaining healthy skin.
Atopic dermatitis is a chronic skin condition with complex causes and significant physical and psychological impacts. Understanding the triggers, symptoms, and available treatments is crucial for effective management. Visiting DermaLinks and consulting our dermatologist is essential for accurate diagnosis, personalized treatment plans, and support in managing the condition. With ongoing research and advancements in treatment options, individuals with atopic dermatitis can look forward to more effective solutions and improved quality of life.
Need Any Help
Request A Consultation And Price Estimate
Seborrhoeic Dermatitis
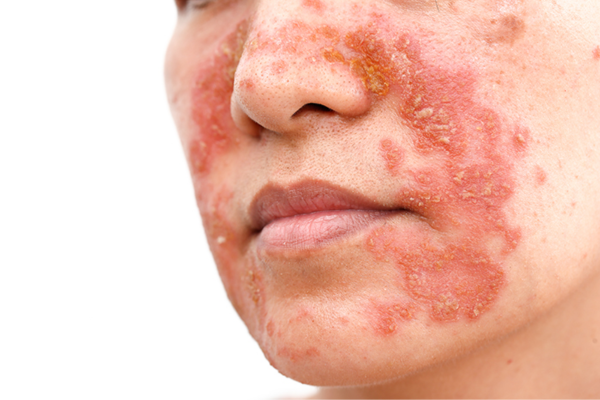
Seborrhoeic dermatitis is a common inflammatory skin condition (type of Eczema) that affects areas of the body with a high density of sebaceous (oil) glands, such as the scalp, face, and upper body. It manifests as red, itchy, and flaky skin. Understanding the causes and effective treatments for seborrhoeic dermatitis is essential for managing this chronic condition.
Possible Causes of Seborrhoeic Dermatitis
- Malassezia Yeast: Overgrowth of the Malassezia yeast, which is naturally present on the skin, is a major factor in seborrhoeic dermatitis.
- Genetics: Family history can increase the likelihood of developing seborrhoeic dermatitis.
- Hormonal Changes: Hormonal fluctuations, such as those occurring during puberty, can trigger or worsen the condition.
- Environmental Factors: Stress, cold weather, and harsh detergents or soaps can exacerbate symptoms.
Symptoms and Diagnosis
- Redness: Red, inflamed skin in seborrhoeic dermatitis-prone areas such as the scalp, face, and upper body.
- Flakiness: White or yellowish flakes, commonly known as dandruff when on the scalp.
- Itching: Persistent itching that can lead to scratching and secondary infections.
- Greasy Skin: Oily patches of skin, often in areas with high sebum production.
- Diagnosis: Dermatologists diagnose seborrhoeic dermatitis through a physical examination and medical history review. In some cases, skin scrapings may be taken to rule out other conditions like psoriasis or fungal infections.
Importance of Visiting DermaLinks
- Accurate Diagnosis: Dermatologist at DermaLinks can accurately diagnose seborrhoeic dermatitis and differentiate it from other similar skin conditions.
- Comprehensive Treatment Plans: Dermatologists can develop individualized treatment plans based on the severity and specific areas affected which may include : Topical Treatments, Medicated shampoo, Oral Medications, Lifestyle changes
- Management of Complications: Dermatologists can manage complications such as secondary bacterial infections or severe inflammation.
- Guidance on Skincare: Dermatologists can offer advice on managing skin symptoms and preventing flare-ups.
Seborrhoeic dermatitis is a common inflammatory skin condition that can significantly impact quality of life. Understanding its causes and effective treatments is essential for managing symptoms and preventing complications. Visiting a dermatologist ensures accurate diagnosis, personalized treatment plans, and access to advanced treatments. With ongoing research and advancements in medical therapies, the future holds promise for improved management of seborrhoeic dermatitis.