Warts
Warts are common benign skin growths caused by infection with the human papillomavirus (HPV). They can appear anywhere on the body and vary in size and appearance depending on the type of HPV involved. Understanding the causes, symptoms, and seeking dermatological advice are essential for managing warts effectively.
Possible Causes of Warts
Warts develop due to infection with HPV, a highly contagious virus that enters the body through small cuts, breaks, or weak spots in the skin. Different types of HPV cause different types of warts:
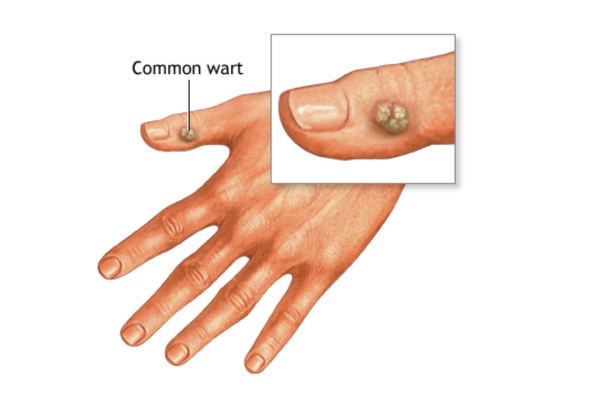
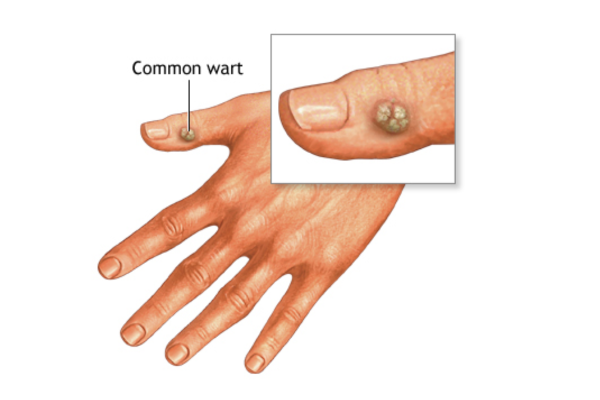
- Common Warts: Typically appear on the hands, fingers, or around the nails. They are often rough, raised, and greyish-brown in colour.
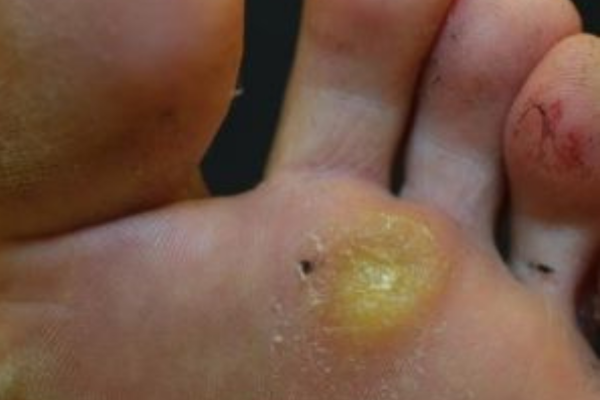
- Plantar Warts: Found on the soles of the feet and can be painful when walking or standing. Plantar warts may have dark spots (petechiae) under the skin’s surface.
- Flat Warts: Smooth, flat-topped, and flesh-colored warts that usually appear on the face, neck, hands, or knees. They may occur in large numbers (up to 100 at a time).
- Genital Warts: Sexually transmitted and appear on the genital and anal areas. Genital warts are caused by specific types of HPV and require medical treatment.
Symptoms and Diagnosis
Warts vary in appearance depending on their location and type:
- Rough Texture: Common warts and plantar warts often have a rough, raised surface.
- Smooth Appearance: Flat warts have a smooth, flat-topped appearance and are usually flesh-colored.
- Clusters: Flat warts and genital warts may appear in clusters and can spread rapidly.
Diagnosis is typically based on a visual examination by a dermatologist, who may perform a skin biopsy or use a dermoscope to examine the wart more closely.
Importance of Visiting DermaLinks
- Accurate Diagnosis: Dermatologists at DermaLinks specialize in diagnosing warts and can differentiate them from other skin lesions or growths, such as moles or skin tags.
- Effective Treatment Options: Dermatologists offer a range of treatments for warts based on their type, location, and severity. Treatment options may include topical medications (such as salicylic acid), cryotherapy (freezing), laser therapy, and surgical removal (excision).
- Prevention of Spread: Professional treatment reduces the risk of spreading warts to other parts of the body or to other people. Dermatologists provide guidance on preventing reinfection and reducing transmission of HPV.
- Monitoring and Follow-up: Dermatologists monitor the response to treatment and provide follow-up care to ensure complete resolution of warts. They may recommend additional treatments or adjustments based on individual response and recurrence of warts.
Warts are benign skin growths caused by infection with HPV. They can appear anywhere on the body and vary in size and appearance depending on the type of HPV involved. Visiting a dermatologist is essential for accurate diagnosis, personalized treatment plans, and effective management to reduce symptoms, prevent spread, and improve skin health.
Need Any Help
Request A Consultation And Price Estimate
Skin tags
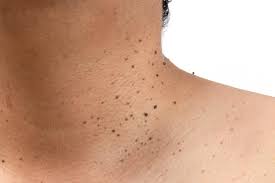
Skin tags are benign, soft, flesh-coloured growths that commonly appear on areas of the body where skin rubs against skin or clothing. They are typically painless and harmless but can be bothersome or cosmetically undesirable. Understanding the causes, symptoms, and seeking dermatological guidance are important for managing skin tags effectively.
Possible Causes of Skin tags
Skin tags develop due to several factors:
- Friction: Skin tags often occur in skin folds or creases where friction or rubbing occurs, such as the neck, armpits, groin, and eyelids.
- Hormonal Changes: Pregnancy and insulin resistance (associated with type 2 diabetes) may increase the likelihood of developing skin tags. Hormonal fluctuations can influence skin cell growth and lead to the formation of skin tags.
- Genetic Predisposition: Family history plays a role in the development of skin tags. Individuals with a family history of skin tags may be more prone to developing them.
- Age: Skin tags are more common in middle-aged and older adults, though they can occur at any age.
Symptoms and Diagnosis
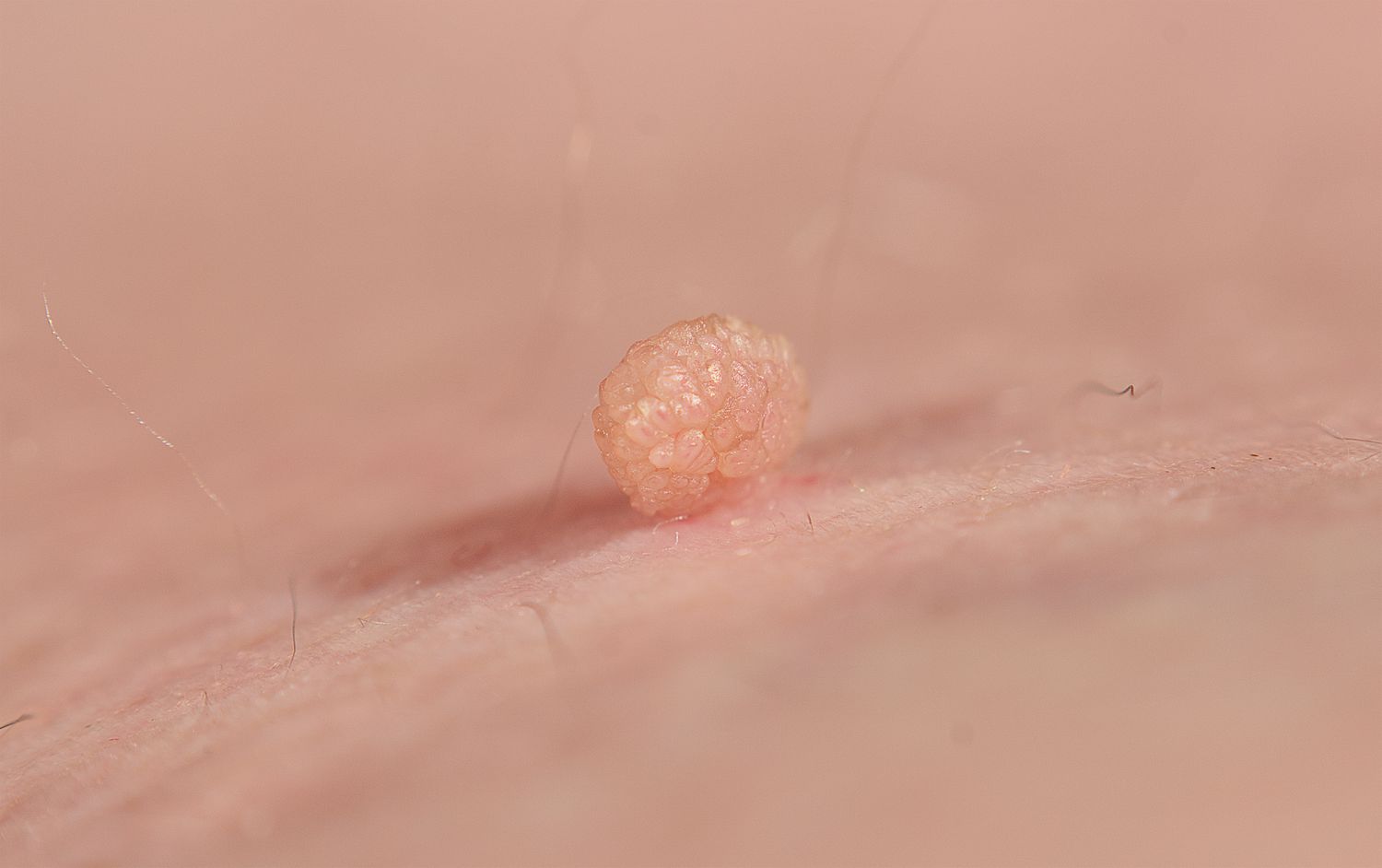
Skin tags are characterized by:
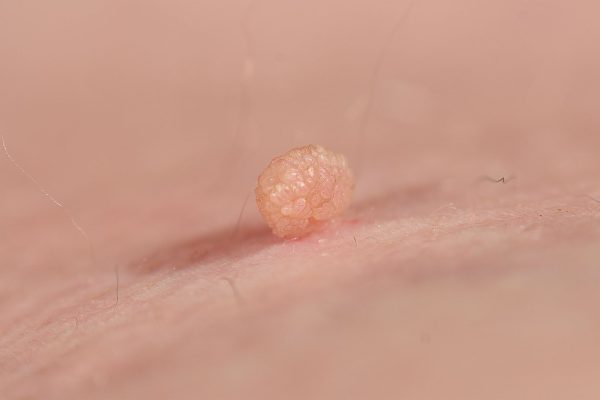
- Small, Soft Growth: Flesh-colored or slightly darker growth that hangs off the skin by a narrow stalk.
- Painless: Skin tags are usually painless but may become irritated if they catch on clothing or jewelry.
- Cosmetic Concerns: Skin tags may be cosmetically bothersome, especially if they appear in visible or sensitive areas.
Diagnosis is typically based on the appearance of the skin growths and may involve a dermatologist visually examining the lesion to confirm that it is a skin tag and not another type of skin lesion.
Importance of Visiting DermaLinks
- Confirmation of Diagnosis: Dermatologists can confirm the diagnosis of skin tags and differentiate them from other skin conditions, such as moles or warts.
- Safe Removal: Dermatologists offer safe and effective methods for removing skin tags, including cryotherapy (freezing), excision (cutting), and cauterization (burning). Professional removal reduces the risk of bleeding, infection, or scarring compared to at-home removal methods.
- Cosmetic Concerns: Skin tags can be cosmetically bothersome, especially if they appear in highly visible or sensitive areas. Dermatologists provide options for removal to address cosmetic concerns and improve skin appearance.
- Prevention of Complications: Professional removal of skin tags reduces the risk of irritation, bleeding, or discomfort associated with untreated or improperly removed skin tags. Dermatologists offer guidance on post-removal care and preventive measures.
Skin tags are benign growths that commonly appear in areas of the body where skin rubs against skin or clothing. They are typically painless but can be cosmetically bothersome. Understanding the causes and seeking dermatological advice are important for accurate diagnosis, safe removal, and prevention of complications. Visiting a dermatologist ensures effective management of skin tags and enhances skin health and appearance.
Need Any Help
Request A Consultation And Price Estimate
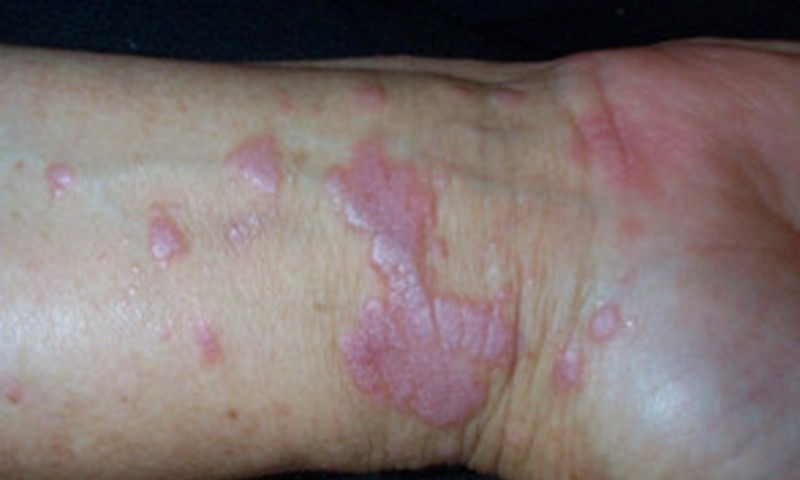
Lichen Planus
Lichen planus is an inflammatory condition that affects the skin, mucous membranes, nails, and hair. It presents as purplish, flat-topped bumps, often accompanied by itching. Understanding the causes and effective treatments for lichen planus is essential for managing this chronic condition and preventing complications.
Possible Causes of Lichen Planus
- Immune System Reaction: Lichen planus is believed to result from an autoimmune response, where the immune system attacks the skin and mucous membranes.
- Genetic Predisposition: Family history can increase the likelihood of developing lichen planus.
- Infections: Viral infections, particularly hepatitis C, are associated with lichen planus.
- Medications: Certain medications, such as nonsteroidal anti-inflammatory drugs (NSAIDs) and beta-blockers, can trigger lichen planus.
Symptoms and Diagnosis
- Symptoms:
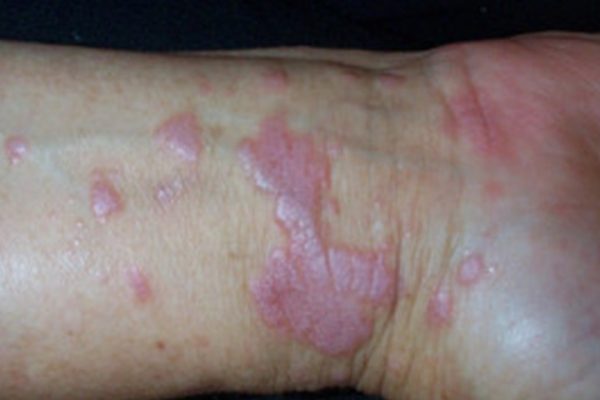
- Skin Lesions: Purplish, flat-topped bumps that can merge into larger patches, often appearing on the wrists, lower back, and ankles.
- Itching: Intense itching is common.
- Mucous Membranes: White, lacy patches in the mouth or on the genitals.
- Nail Changes: Thinning, ridging, and splitting of the nails.
- Hair Loss: Scalp involvement can lead to hair loss.
- Diagnosis: Dermatologists diagnose lichen planus through a physical examination, medical history review, and a skin biopsy to confirm the diagnosis and rule out other conditions.
Importance of Visiting DermaLinks
- Accurate Diagnosis: Dermatologists at DermaLinks can accurately diagnose lichen planus and differentiate it from other skin conditions.
- Comprehensive Treatment Plans: Dermatologists can develop individualized treatment plans based on the severity and specific areas affected which may include Topical treatments, Oral medications, Phototherapy and Lifestyle medications.
- Management of Complications: Dermatologists can manage complications such as oral lichen planus and potential secondary infections.
- Guidance on Skincare: Dermatologists can offer advice on managing skin symptoms and preventing flare-ups.
Need Any Help
Request A Consultation And Price Estimate
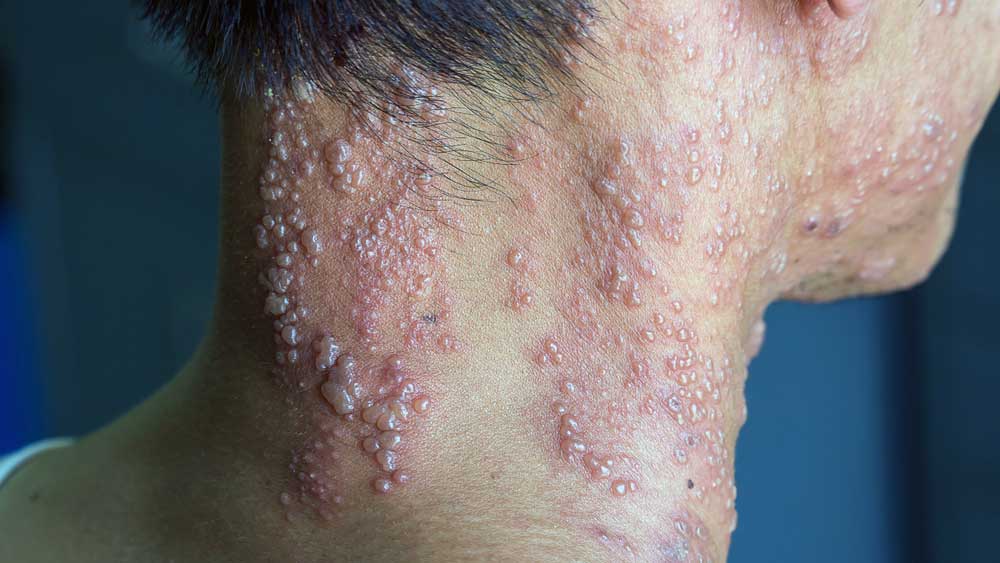
Herpes Zoster
Lichen planus is an inflammatory condition that affects the skin, mucous membranes, nails, and hair. It presents as purplish, flat-topped bumps, often accompanied by itching. Understanding the causes and effective treatments for lichen planus is essential for managing this chronic condition and preventing complications.
Possible Causes of Herpes Zoster
- Varicella-Zoster Virus Reactivation: After an individual recovers from chickenpox, the virus remains dormant in the nerve tissue. Years later, it can reactivate as shingles.
- Weakened Immune System: Factors such as aging, illness, or immune-suppressing treatments can weaken the immune system, increasing the risk of shingles.
- Stress: Physical or emotional stress can contribute to the reactivation of the virus.
- Medications: Certain medications, particularly those that suppress the immune system, can trigger shingles.
Symptoms and Diagnosis
- Symptoms:
- Pain: Often the first symptom, ranging from mild to severe, occurring before the rash.
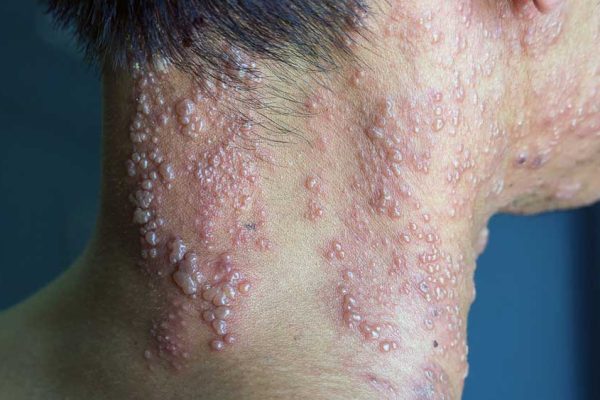
- Rash: A red rash that develops into fluid-filled blisters.
- Itching: Intense itching around the affected area.
- Fever and Malaise: Low-grade fever, headache, and general discomfort.
- Diagnosis: Dermatologists diagnose herpes zoster through a physical examination of the rash and blisters. Lab tests, such as PCR or viral culture, can confirm the diagnosis.
Importance of Consulting at DermaLinks
- Accurate Diagnosis: Dermatologists can accurately diagnose shingles, distinguishing it from other skin conditions.
- Timely Treatment: Early treatment with antiviral medications can reduce the severity and duration of symptoms and prevent complications. Common Treatments may include Antiviral medications, Pain Management Medications, Topical Treatments etc.
- Management of Complications: Dermatologists at DermaLinks can manage complications such as postherpetic neuralgia (PHN) and secondary bacterial infections.
- Preventive Measures: Dermatologists can advise on vaccination and other preventive measures.
Herpes zoster is a painful condition resulting from the reactivation of the varicella-zoster virus. Understanding its causes, symptoms, and treatments is essential for effective management. Visiting a dermatologist ensures accurate diagnosis, timely treatment, and management of complications. With advances in vaccines and antiviral therapies, the future holds promise for improved prevention and treatment of shingles.
Need Any Help
Request A Consultation And Price Estimate
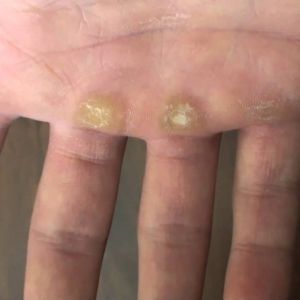
Callosities and Corns
Callosities, commonly known as calluses, and corns are thickened and hardened areas of the skin that develop as a result of repeated friction, pressure, or other forms of irritation. They are most commonly found on the hands, feet, and other areas subject to frequent rubbing. Although callosities and corns are generally not harmful, they can become painful and uncomfortable if left untreated. Understanding their differences, causes, symptoms, and the importance of seeking professional care is crucial for effective management.
Callosities (Calluses)
- Size and Shape: Calluses are larger, more diffuse areas of thickened skin.
- Location: Commonly found on weight-bearing areas such as the soles of the feet and palms of the hands.
- Symptoms: Usually less painful than corns, with a rough texture and a yellowish or grey color.
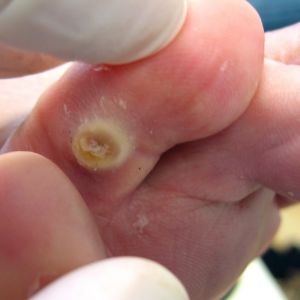
Corns
- Size and Shape: Corns are smaller, rounder, and more defined areas of thickened skin with a central core.
- Location: Typically develop on the toes and areas of the feet subject to direct pressure.
- Symptoms: More painful than calluses, especially when pressure is applied, with redness and inflammation around the corn.
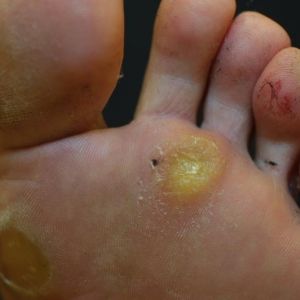
Possible Causes of Callosities and Corns
- Repetitive Friction and Pressure: Continuous friction and pressure from activities such as walking, running, playing musical instruments, or manual labor can cause the skin to thicken and form callosities and corns.
- Ill-Fitting Footwear: Shoes that are too tight, too loose, or have high heels can create pressure points and contribute to the development of both calluses and corns on the feet.
- Abnormal Foot Structure: Conditions such as bunions, hammertoes, and other foot deformities can lead to uneven distribution of pressure, resulting in callosities and corns.
- Occupational Hazards: Certain occupations that involve repetitive hand movements or prolonged standing can increase the risk of developing calluses and corns.
- Barefoot Walking: Walking barefoot, especially on rough surfaces, can lead to the formation of calluses and corns on the soles of the feet.
Symptoms and Diagnosis
Symptoms of Callosities
- Thickened Skin: Areas of thickened, hardened skin that may be yellowish or grey in color.
- Rough Texture: The affected area often feels rough to the touch.
- Pain and Discomfort: Callosities can become painful, especially when pressure is applied.
- Cracks and Fissures: In severe cases, calluses can develop cracks and fissures, which can be painful and increase the risk of infection.
Symptoms of Corns
- Thickened Skin: Small, round areas of thickened, hardened skin, often with a central core.
- Pain and Discomfort: Corns can be painful, especially when pressure is applied.
- Redness and Inflammation: The skin around the corn may become red and inflamed.
- Tenderness: Corns are often tender to the touch.
Diagnosis
Dermatologists diagnose callosities and corns through a physical examination of the affected area. They may also ask about the patient’s medical history, lifestyle, and activities to determine the underlying cause.
Importance of Consulting at DermaLinks
Accurate Diagnosis
Differentiation: Dermatologists at DermaLinks can differentiate callosities and corns from other skin conditions, such as warts and plantar keratosis, which may require different treatments.
Comprehensive Treatment Plans
Personalized Care: Dermatologists can develop individualized treatment plans to address the specific needs and underlying causes of callosities and corns. Common treatment solutions include:
- Topical Treatments: Use of medicated creams to soften thickened skin.
- Physical Treatments: Paring down thickened skin using specialized tools.
- Medical Procedures: Laser therapy or minor surgical procedures for severe cases.
- Lifestyle Changes: Advice on proper footwear and foot care practices.
Prevention of Complications
Monitoring and Treatment: Regular monitoring and treatment by a dermatologist can prevent complications such as infections, ulcers, and further skin damage.
Education and Support
Foot Care Guidance: Dermatologists can provide valuable information on proper foot care, footwear, and lifestyle modifications to prevent the recurrence of callosities and corns.
Callosities and corns are common skin conditions that develop as a result of repeated friction and pressure. While callosities are larger and generally less painful, corns are smaller, more painful, and have a central core. Understanding the underlying causes, symptoms, and available treatments is crucial for effective management. Consulting dermatologists at DermaLinks is essential for accurate diagnosis, personalized treatment plans, and prevention of complications. With ongoing research and advancements in treatment options, individuals with callosities and corns can look forward to more effective solutions and improved quality of life.
Need Any Help
Request A Consultation And Price Estimate

Macular Amyloidosis
Macular amyloidosis is a skin condition characterized by the appearance of small, itchy brown patches on the skin. These patches typically develop on the upper back, chest, and arms, though they can occur elsewhere on the body. While the exact cause of macular amyloidosis is not fully understood, it is believed to involve the deposition of amyloid proteins in the skin layers. This condition primarily affects adults and is more commonly seen in individuals with darker skin tones, particularly those of Asian, Middle Eastern, or Latin American descent.
Possible Causes
The precise cause of macular amyloidosis remains unclear, but several factors are thought to contribute to its development:
- Genetic Predisposition: There appears to be a genetic predisposition to macular amyloidosis, with familial clustering observed in some cases.
- Environmental Factors: Chronic friction or rubbing of the skin is believed to play a role in the development of amyloid deposits. This friction may result from activities like scratching or wearing tight clothing.
- Ethnicity: Macular amyloidosis is more commonly observed in individuals of Asian, Middle Eastern, and Latin American descent, suggesting a possible ethnic predisposition.
- Gender: Women are more frequently affected by macular amyloidosis than men, though the reasons for this gender disparity are not well understood.
Symptoms and Diagnosis
Macular amyloidosis typically presents as small, flat, brownish patches on the skin. These patches may be slightly raised and can feel itchy or irritated, particularly after friction or scratching. Diagnosis is usually made based on the characteristic appearance of the skin lesions and may involve a skin biopsy to confirm the presence of amyloid deposits.
Importance of Visiting DermaLinks
- Accurate Diagnosis: Dermatologists at DermaLinks specialize in diagnosing skin conditions and can differentiate macular amyloidosis from other skin disorders that may appear similar.
- Treatment Options: While macular amyloidosis may not always require treatment, dermatologists can provide options to alleviate symptoms such as itching and discomfort. These may include topical corticosteroids, emollients, or antihistamines.
- Monitoring and Management: Regular visits to a dermatologist ensure ongoing monitoring of the condition. Dermatologists can assess the progression of macular amyloidosis and recommend appropriate interventions if necessary.
- Prevention of Complications: Early intervention by a dermatologist can help prevent complications such as secondary infections due to scratching or irritation of the skin.
Summary
Macular amyloidosis is a benign skin condition characterized by brownish patches that can be itchy and irritating. While the exact cause is uncertain, factors such as genetics, ethnicity, and environmental factors may contribute to its development. Visiting a dermatologist is crucial for accurate diagnosis, symptom management, and monitoring of the condition to ensure optimal skin health.